Commentary by EAS Scientific writer Jane K. Stock
A European Atherosclerosis Society Task Force has focused on rare dyslipidaemias in this latest statement, published in Lancet Diabetes & Endocrinology. Although these disorders affect few individuals, collectively they pose a substantial burden to patients, their families and healthcare systems. The Task Force highlights the need for collaborative registries to address the lack of information for many of these disorders.
Rare dyslipidaemias: why new focus is needed
Due to their rarity, rare lipoprotein disorders are largely under-recognised and undertreated. This is not surprising, as given their infrequency, clinicians may only see one or two affected people in their entire careers and misdiagnosis is therefore common. Furthermore, the fact that there are currently very few disease-specific rare lipoprotein disorder patient registries, means that there is a scarcity of quality information about the prevalence, pathophysiology, and outcomes of these disorders. Evidence-based clinical management of these conditions is therefore problematic.
Although rare lipoprotein disorders affect only a few individuals (by definition, a rare disease affects 40–50 cases per 100 000 people1,2), the burden posed to patients and their families, as well as all in the care pathway, is substantial, when considering the associated disability and morbidity. The fragmented nature of epidemiologic information relating to these conditions is a key deterrent affecting the development of evidence-based service planning.
Most of these conditions have a genetic component. Advances in genomics and DNA sequencing, means that genetic testing for these conditions is now more readily available and less expensive. Despite this, a key concern for clinicians is whether genetic testing is a prerequisite for diagnosis and management of all patients with rare dyslipidaemias.
A public health response to rare dyslipidaemias needs a framework to operate in a coordinated manner. It is evident that accessible clinical guidance is much needed in this area. This new consensus statement from the European Atherosclerosis Society (EAS) provides important scientific background, and a pragmatic practical guide to definitive diagnosis and treatment.3
Scope of the Task Force statement
This Task Force statement provides an overview of the underlying pathophysiology, and clinical guidance for rare lipoprotein disorders associated with extreme levels (either low or high) of low-density lipoprotein cholesterol (LDL-C), triglycerides and high-density lipoprotein cholesterol (HDL-C). Familial hypercholesterolaemia (heterozygous FH) is not covered in this statement as it is not a rare disorder (by either European or USA definitions1,2), affecting one individual in 200-250 people,4,5 but homozygous FH, which is rare, is discussed. The information presented complements and updates a previous EAS Consensus Panel statement on homozygous FH.6
Rare lipoprotein disorders characterised by extremely high or low LDL-C levels
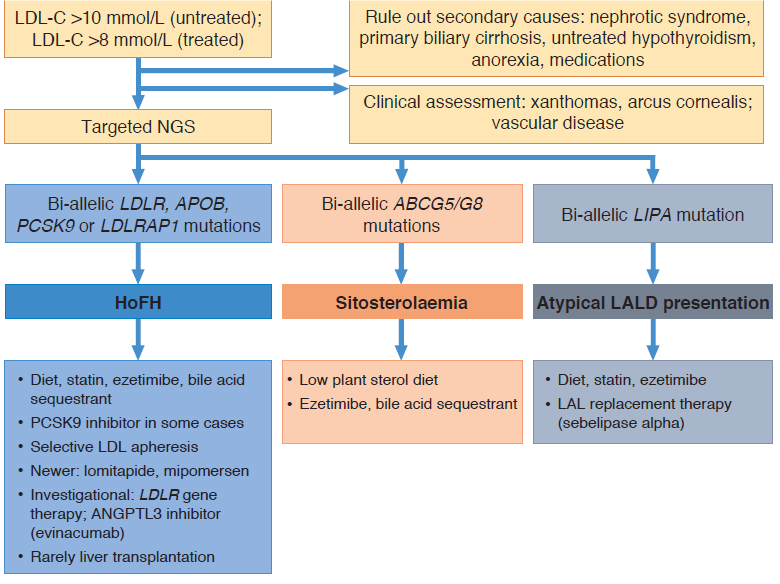
Very high LDL-C: Homozygous FH is the predominant lipoprotein disorder discussed in the phenotypic context of very high LDL-C levels. Recent insights have led to a re-examination of the terminology of this disorder, with recognition of its heterogeneity in respect of causative genetic loci, as well as polygenic aetiology.3,7 The Task Force emphasises that although genetic testing may be helpful in differentiating other rare dyslipidaemia with a similar clinical presentation, notably 1) β-sitosterolaemia (phytosterolaemia), an autosomal recessive disorder due to mutations in the ABCG5 and ABCG8 genes, and 2) lysosomal acid lipase deficiency, an autosomal recessive disorder of the LIPA gene, it is the plasma LDL-C concentration rather than genetic aetiology that is the main guide to the clinical management of homozygous FH (Figure 1). Treatment of homozygous FH typically comprises the combination of maximally tolerated statin, ezetimibe and a PCSK9 inhibitor, in addition to diet and lifestyle, as well as lipoprotein apheresis.6,8 Genetic insights have been a driver for novel adjunctive treatments, including evinacumab (a monoclonal antibody to ANGPTL3) and LDLR gene therapy.9,10
Figure 1. Management of rare lipoprotein disorders characterised by very high LDL-C levels
Abbreviations: ANGPTL3 angiopoietin-like 3; HoFH homozygous familial hypercholesterolaemia; NGS next generation sequencing; PCSK9 proprotein convertase subtilisin/kexin type 9.
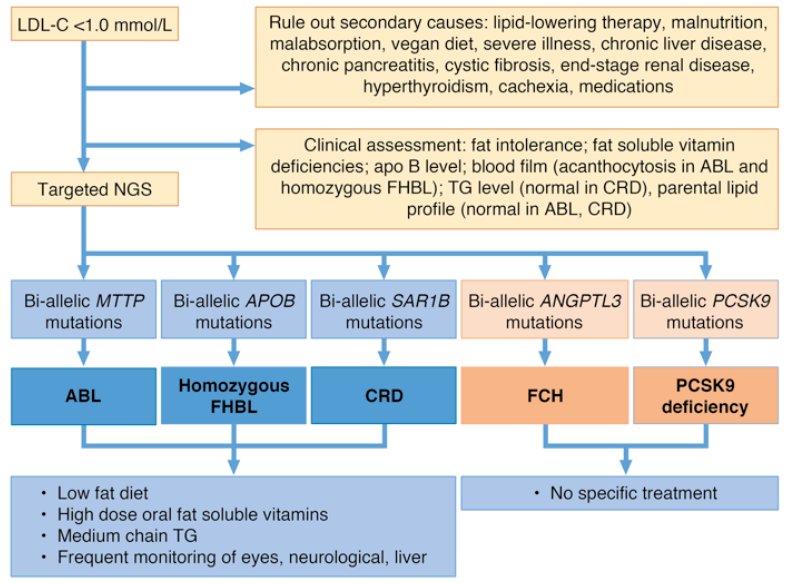
Very low LDL-C levels: Rare lipoprotein disorders causing primary hypobetalipoproteinaemia (characterised by very low LDL-C levels) involve mutations in five defined genes. Loss-of-function mutations in the MTTP gene, encoding microsomal triglyceride transfer protein, cause abetalipoproteinaemia, which is characterised by undetectable plasma levels of LDL-C and apolipoprotein (apo) B, as well as very low levels of triglycerides and total cholesterol. Homozygous familial hypobetalipoproteinaemia, an autosomal co-dominant disorder involving the APOB gene, is typically characterised by LDL-C levels <1.0 mmol/L (<38·7 mg/dL). Other disorders characterised by primary hypobetalipoproteinaemia are 1) chylomicron retention disease, caused by loss-of-function mutations in SAR1B, the gene encoding Sar1 homolog B GTPase; 2) familial combined hypolipidaemia, caused by mutations in ANGPTL3; and 3) PCSK9 deficiency. Fat intolerance and deficiencies in fat-soluble vitamin deficiencies are characteristic of all these disorders; measurement of triglycerides can help to differentiate chylomicron retention disease (normal levels) from the other disorders. In addition, a normal lipid profile is parents is a characteristic of abetalipoproteinaemia and chylomicron retention disease, and therefore an aid to differential diagnosis.
The cornerstones of treatment for abetalipoproteinaemia, homozygous familial hypobetalipoproteinaemia and chylomicron retention disease are a low-fat diet (with or without medium chain triglycerides) together with supplementation with essential fatty acids and high-dose vitamins A, D, E, and K. No treatment is indicated for hypobetalipoproteinaemia associated with ANGPTL3 or PCSK9 loss-of-function mutations (Figure 2).
Figure 2. Management of rare lipoprotein disorders characterised by very low LDL-C levels
Abbreviations: ABL abetalipoproteinaemia; CRD chylomicron retention disease; FCH familial combined hyperlidaemia; FHBL familial hypobetalipoproteinaemia; TG triglycerides.
Rare lipoprotein disorders characterised by extremely high or low triglycerides
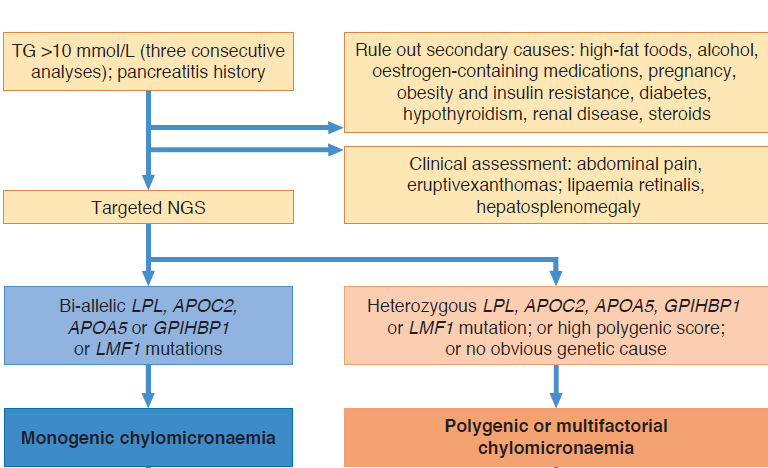
Very high triglycerides: In the context of this statement, a very high triglyceride level is defined as >10 mmol/L (>885 mg/dL), differentiating this from hypertriglyceridaemia commonly encountered in the clinic (>2.0 mmol/L or >180 mg/dL). The Task Force emphasises that severe hypertriglyceridemia is primarily polygenic, as less than 0.1-0.2% of individuals have a monogenic aetiology. In these patients, genes that play a role in regulating triglyceride-rich lipoprotein metabolism are implicated, i.e. LPL (encoding lipoprotein lipase; LPL), APOC2 (encoding apo C-II), APOA5 (encoding apo A-V), LMF1 (encoding lipase maturation factor 1), and GPIHBP1 (encoding glycosylphosphatidylinositol-anchored HDL binding protein 1).11-14 The preferred terminology is monogenic chylomicronaemia (alternatively referred to as familial chylomicronaemia syndrome).
In contrast with individuals with multifactorial or likely polygenic aetiologies, those with monogenic chylomicronaemia tend to present with elevated triglycerides (typically >20 mmol/L) at a much younger age, are less likely to be obese or have secondary factors, are at higher lifetime risk of acute pancreatitis, and are very resistant to triglyceride-lowering pharmacotherapy (Figure 3). Other proposed monogenic causes of severe hypertriglyceridaemia are discussed.
Figure 3. Diagnosis of severe hypertriglyceridaemia
The foundation of therapy of severely elevated triglycerides is a low-fat diet (with medium chain fatty acids), avoidance of alcohol, and reduced intake of high glycaemic food; fibrates and omega-3 fatty acids can be effective in individuals with polygenic chylomicronaemia but not in those with monogenic chylomicronaemia. Adherence with these dietary requirements is, however, problematic for most patients. The risk of pancreatitis is a key issue, as is the need for more effective therapy. Genetic insights have been a driver for the development of novel pharmacotherapies targeting apo C-III (antisense oligonucleotides) or ANGPTL3 (monoclonal antibody and an antisense oligonucleotide).
Very low triglycerides: The Task Force notes that no single gene disorder lowers triglycerides exclusively; this presentation is a feature of multisystem disorders characterised by low or undetectable apo B-containing lipoproteins.
Rare lipoprotein disorders characterised by high or low HDL-C levels
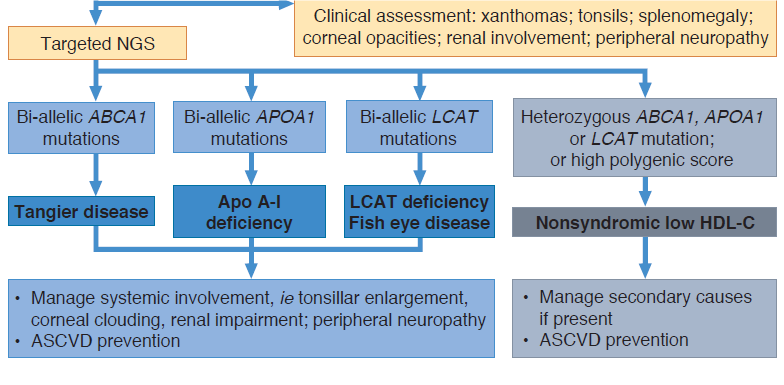
Very low HDL-C levels: Secondary factors (see Table) may be implicated in up to half of individuals with very low HDL-C levels (<0.5 mmol/L or <20 mg/dL);15 after exclusion, mutations in key genes involved in the biogenesis of HDL, APOA1, ABCA1, LCAT, or LPL, may be causative in those with an identified genetic basis, although others may have a polygenic cause. Specific clinical features can be an aid to diagnosis; management of disorders associated with very low HDL-C levels are summarised in Figure 4. Currently, there is no specific treatment for apolipoprotein A-I deficiency, Tangier disease and LCAT deficiency syndromes. Treatments investigated to date include infusion of synthetic HDL in patients with apolipoprotein A-I deficiency or Tangier disease16; and enzyme replacement therapy with human recombinant LCAT and small molecules enhancing LCAT activity (LCAT deficiency syndromes).17,18
Table. Secondary causes of low HDL cholesterol
| Very low HDL cholesterol (<0.5 mmol/L) | Moderately low HDL cholesterol (<0.5-0.9 mmol/L) | |
| Underlying diseases | • Severe hypertriglyceridaemia • Uncontrolled diabetes • Liver failure (acute hepatic failure, congested liver/right heart failure, primary biliary liver cirrhosis) • Systemic / acute inflammation • Haemato-oncological diseases (acute lymphoblastic leukaemia, chronic myelogenous leukaemia, multiple myeloma) | • Moderate hypertriglyceridaemia • Type 2 diabetes mellitus • Obesity • Chronic inflammation • Growth hormone excess • Hypercortisolism • Chronic kidney disease |
| Lifestyle | N/A | • Smoking • Physical inactivity |
| Life style, drugs | • Androgens (testosterone, anabolic drugs) • Probucol | • Thiazide diuretics • Some beta-blockers • Anti-retroviral drugs |
Figure 4. Diagnosis and management of low HDL-C (<0.5 mmol/L or <20 mg/dL)
Abbreviation: ASCVD atherosclerotic cardiovascular disease
Very high HDL-C levels: Elevated HDL-C levels, typically exceeding 2.6 mmol/L (100 mg/dL), are associated with loss-of-function mutations in CETP, encoding cholesteryl ester transfer protein, and SRB1, encoding scavenger receptor B-I. Rarely, loss-of function mutations in the LIPC gene are also implicated; this disorder is also characterised by hypercholesterolaemia, hypertriglyceridaemia, and an increase in compositionally abnormal HDL. Management of this disorder is aimed at reducing the risk of atherosclerotic cardiovascular disease.
Conclusion
This latest EAS statement is timely given the pace of recent progress in genomic research. It provides pragmatic clinical guidance for patients with these rare dyslipidaemias, who ideally should be managed in specialised centres. There are, however, outstanding questions critical to improving patient management. Notably, will advances in molecular technologies lead to improved access and reduced cost of diagnostic approaches? And will genomic insights translate to novel therapies for those rare lipoprotein disorders with limited therapeutic options? The Task Force recognises that a key deterrent is the limited information relating to the prevalence, pathophysiology, and outcomes for these rare disorders. National and international registries are much needed to address these deficiencies, to drive future rare disease research efforts, facilitate clinical trials of new therapies, and ultimately improve patient outcomes. Collaboration between all stakeholders in the care pathway, and patients and their families is essential for this to become reality.
References
1. European Medicines Agency. Orphan designation: overview. https://www.ema.europa.eu/en/human-regulatory/overview/orphan-designation-overview (accessed April 4, 2019).
2. Orphan Drug Act. Rare diseases act of 2002. https://www.govinfo.gov/content/pkg/PLAW-107publ280/html/PLAW-107publ280.htm (accessed April 4, 2019).
3. Hegele RA, Borén J, Ginsberg HN, Arca M, Averna M, Binder CJ, Calabresi L, Chapman MJ, Cuchel M, von Eckardstein A, Frikke-Schmidt R, Gaudet D, Hovingh GK, Kronenberg F, Lütjohann D, Parhofer KG, Raal FJ, Ray KK, Remaley AT, Stock JK, Stroes ES, Tokgözoğlu L, Catapano AL. Rare dyslipidaemias, from phenotype to genotype to management: a European Atherosclerosis Society task force consensus statement. Lancet Diabetes Endocrinol 2019; doi: 10.1016/S2213-8587(19)30264-5. Link: https://www.thelancet.com/journals/landia/article/PIIS2213-8587(19)30264-5/fulltext
4. Benn M, Watts GF, Tybjærg-Hansen A, Nordestgaard BG. Mutations causative of familial hypercholesterolaemia: screening of 98 098 individuals from the Copenhagen General Population Study estimated a prevalence of 1 in 217. Eur Heart J 2016;37:1384-94.
5. Do R, Stitziel NO, Won HH et al. Exome sequencing identifies rare LDLR and APOA5 alleles conferring risk for myocardial infarction. Nature 2015;518:102-6.
6. Cuchel M, Bruckert E, Ginsberg HN et al. Homozygous familial hypercholesterolaemia: new insights and guidance for clinicians to improve detection and clinical management. A position paper from the Consensus Panel on Familial Hypercholesterolaemia of the European Atherosclerosis Society. Eur Heart J 2014;35:2146-57.
7. Berberich AJ, Hegele RA. The complex molecular genetics of familial hypercholesterolaemia. Nat Rev Cardiol 2019;16:9-20.
8. Julius U. Current role of lipoprotein apheresis in the treatment of high-risk patients. J Cardiovasc Dev Dis 2018; 5: e27.
9. Hegele RA, Tsimikas S. Lipid-lowering agents. Circ Res 2019; 124: 386–404.
10. Gaudet D, Gipe DA, Pordy R, et al. ANGPTL3 inhibition in homozygous familial hypercholesterolemia. N Engl J Med 2017;377: 296–97.
11. Brahm AJ, Hegele RA. Chylomicronaemia—current diagnosis and future therapies. Nat Rev Endocrinol 2015; 11: 352–62.
12. Dron JS, Wang J, Cao H, et al. Severe hypertriglyceridemia is primarily polygenic. J Clin Lipidol 2019; 13: 80–88.
13. Dron JS, Hegele RA. Genetics of triglycerides and the risk of atherosclerosis. Curr Atheroscler Rep 2017; 19: 31.
14. Hegele RA, Berberich AJ, Ban MR, et al. Clinical and biochemical features of different molecular etiologies of familial chylomicronemia. J Clin Lipidol 2018; 12: 920–27.
15. Geller AS, Polisecki EY, Diffenderfer MR, et al. Genetic and secondary causes of severe HDL deficiency and cardiovascular disease. J Lipid Res 2018; 59: 2421–35.
16. Kootte RS, Smits LP, van der Valk FM, et al. Effect of open-label infusion of an apoA-I-containing particle (CER-001) on RCT and artery wall thickness in patients with FHA. J Lipid Res 2015;56: 703–12.
17. Shamburek RD, Bakker-Arkema R, Shamburek AM, et al. Safety and tolerability of ACP-501, a recombinant human lecithin: cholesterol acyltransferase, in a phase 1 single-dose escalation study. Circ Res 2016; 118: 73–82.
18. Freeman LA, Demosky SJ Jr, Konaklieva M, et al. Lecithin: cholesterol acyltransferase activation by sulfhydryl-reactive small molecules: role of cysteine-31. J Pharmacol Exp Ther 2017;362: 306–18.